Current medical research shows that nuts, seeds, and popcorn DO NOT trigger diverticulitis flares as previously believed. During active flare-ups, doctors recommend a temporary low-fiber diet including clear liquids, broths, and refined grains. Long-term prevention focuses on high-fiber foods like fruits, vegetables, and whole grains - but individual triggers vary significantly.
Understanding Diverticulitis Triggers: What Science Says Today
If you've recently experienced diverticulitis pain or received a diagnosis, you're probably searching for clear answers about which foods to avoid. This confusion is understandable - dietary recommendations have dramatically shifted in recent years as medical research has evolved. Let's cut through the misinformation with evidence-based guidance you can trust.
Diverticulitis 101: Separating Fact from Fiction
Diverticulitis occurs when small pouches (diverticula) in your colon become inflamed or infected. For decades, doctors advised patients to avoid nuts, seeds, and popcorn, fearing these foods would get trapped in the pouches and cause inflammation. However, multiple large-scale studies have completely debunked this theory.
According to the American Gastroenterological Association's 2023 clinical guidelines, "there is no evidence that nut, seed, or popcorn consumption increases the risk of diverticulitis or diverticular bleeding." This represents a major shift from previous recommendations.
How Dietary Recommendations Have Evolved: A Medical Timeline
The understanding of diverticulitis triggers has changed dramatically over the past 20 years. This timeline shows how medical consensus has evolved based on new research:
| Time Period | Common Recommendation | Current Medical View |
|---|---|---|
| 1990s-2000s | Avoid all nuts, seeds, popcorn, and high-fiber foods | Outdated - no scientific basis |
| 2010-2018 | Gradual reintroduction of fiber; still caution with seeds/nuts | Partially updated but still overly restrictive |
| 2019-Present | High-fiber diet recommended for prevention; no restrictions on nuts/seeds | Current standard of care per AGA guidelines |
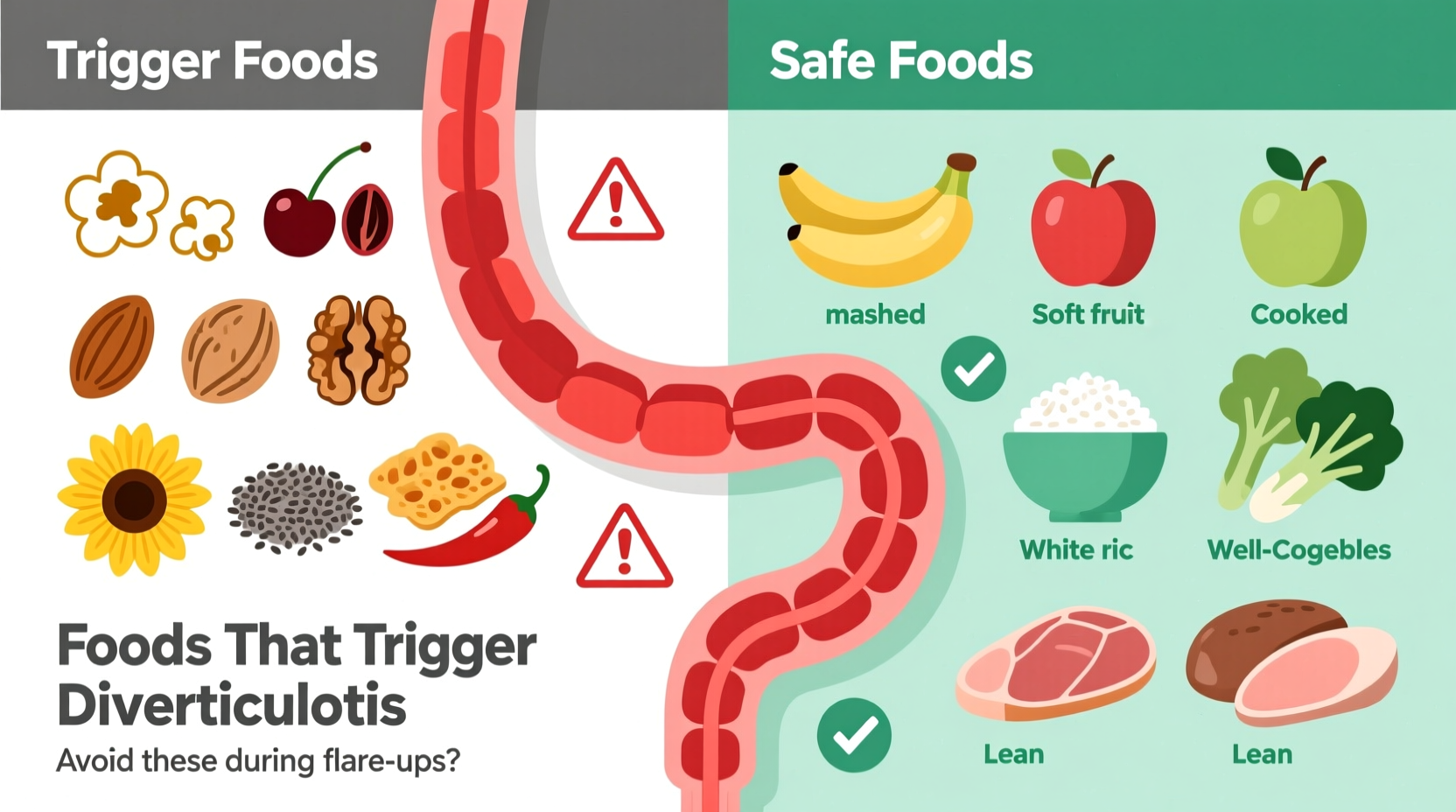
Foods to Limit During Active Flare-Ups (Short-Term)
When experiencing acute diverticulitis symptoms, your doctor will likely recommend a temporary low-fiber diet to allow your colon to heal. This typically lasts 2-4 days and includes:
- Clear liquids: broth, apple juice, gelatin
- Refined grains: white rice, white bread, pasta
- Cooked vegetables without skin
- Easily digestible proteins: eggs, fish, chicken
As symptoms improve, you'll gradually reintroduce fiber under medical supervision. The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) emphasizes that this short-term restriction is not a permanent dietary change.
Foods That Support Long-Term Prevention
For preventing future diverticulitis episodes, research consistently shows that a high-fiber diet is protective. The Journal of Gastroenterology published a 2022 meta-analysis confirming that diets rich in fruits, vegetables, and whole grains reduce diverticulitis recurrence by up to 35%.
Focus on incorporating these evidence-backed foods:
- Fruits: Berries, apples (with skin), pears, oranges
- Vegetables: Broccoli, Brussels sprouts, carrots, sweet potatoes
- Whole grains: Oatmeal, brown rice, quinoa, whole-wheat bread
- Legumes: Lentils, black beans, chickpeas (introduced gradually)
- Nuts and seeds: Almonds, walnuts, chia seeds, flaxseeds (no restriction needed)

Individual Triggers: Why Your Experience May Differ
While medical guidelines provide general recommendations, individual responses vary. Some people report specific triggers that don't align with current research. This variation is normal and highlights why personalized medical guidance is essential.
Commonly reported individual triggers include:
- Spicy foods (for some individuals)
- High-fat foods during recovery
- Carbonated beverages
- Alcohol (particularly during active flares)
The key is tracking your personal responses. The American College of Gastroenterology recommends keeping a detailed food diary for 4-6 weeks to identify your unique triggers while following your doctor's overall guidance.
Practical Meal Planning Strategies
Transitioning to a diverticulitis-friendly diet doesn't have to be complicated. Try these evidence-based approaches:
- Gradual fiber increase: Add 5 grams of fiber weekly to avoid bloating
- Hydration focus: Drink 8 glasses of water daily when increasing fiber
- Smart food prep: Peel and cook vegetables during recovery, then transition to raw
- Meal timing: Smaller, more frequent meals reduce digestive stress
Remember that consistency matters more than perfection. A 2023 study in Clinical Gastroenterology found that patients who maintained an 80% adherence to high-fiber recommendations saw significant benefits compared to those following restrictive diets.
When to Consult Your Healthcare Provider
Dietary changes alone cannot treat active diverticulitis. Seek immediate medical attention if you experience:
- Severe abdominal pain (especially left lower quadrant)
- High fever or chills
- Rectal bleeding
- Inability to tolerate liquids
Your doctor may recommend antibiotics, pain management, or in severe cases, hospitalization. Never self-treat acute diverticulitis with dietary changes alone.
Building Your Personalized Diverticulitis Diet Plan
The most effective approach combines medical guidance with personal observation. Work with your healthcare provider to develop a plan that includes:
- Short-term low-fiber diet during flares
- Gradual reintroduction of fiber as symptoms improve
- Long-term high-fiber eating pattern for prevention
- Personalized trigger identification through food journaling
Remember that diverticulosis (having diverticula) is extremely common and usually asymptomatic. Developing diverticulitis is not inevitable, and proper dietary management significantly reduces recurrence risk according to the latest research from the Mayo Clinic Proceedings.










 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4