Many people search for 'cauliflower warts' when they notice unusual skin growths. This common misnomer actually describes genital warts that develop a distinctive cauliflower-like appearance as they grow. Understanding this condition begins with recognizing it's not a separate medical condition but rather a visual description of certain genital warts.
What Medical Professionals Call 'Cauliflower Warts'
When healthcare providers examine what patients describe as 'cauliflower warts,' they're typically diagnosing condyloma acuminata—a manifestation of human papillomavirus (HPV) infection. The Centers for Disease Control and Prevention (CDC) identifies HPV types 6 and 11 as responsible for 90% of these cases (CDC, 2023).
Unlike common warts on hands or feet, these growths develop in moist genital areas and take their name from their distinctive appearance. As individual warts cluster together, they form raised, irregular bumps resembling cauliflower florets.
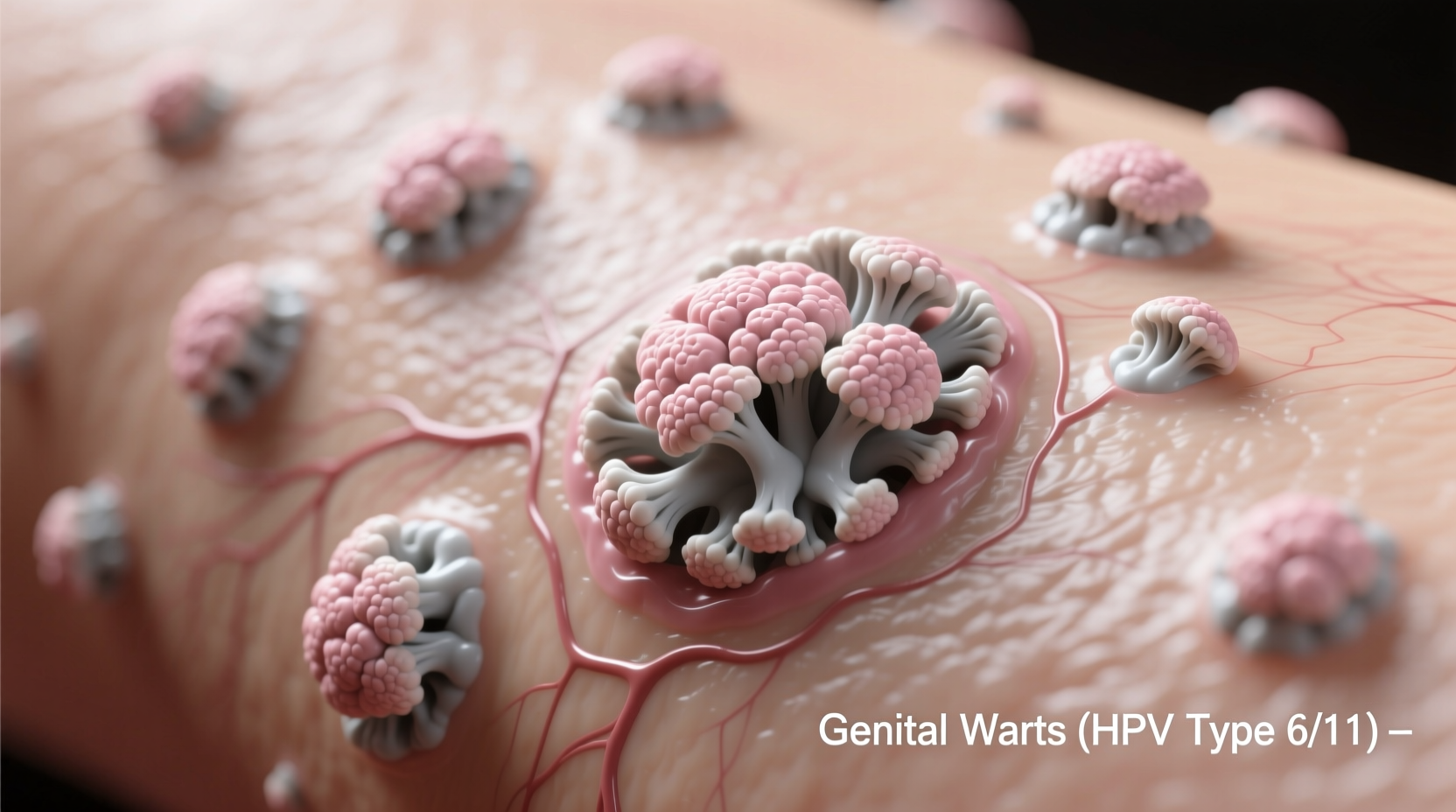
Symptoms and Development Timeline
Understanding the progression helps identify these growths early:
| Stage | Timeframe | Characteristics |
|---|---|---|
| Initial infection | 2 weeks-2 months | No visible symptoms; virus establishes itself |
| Early growth | 1-3 months | Small, flesh-colored bumps appear |
| Cluster formation | 3-6 months | Bumps multiply, creating cauliflower texture |
| Mature presentation | 6+ months | Distinct cauliflower-like clusters |
Most people notice the first small bumps within 2-3 months after exposure. The CDC reports that approximately 360,000 Americans develop genital warts annually (CDC STI Statistics).
Transmission and Risk Factors
HPV spreads through skin-to-skin contact during sexual activity. Key transmission facts:
- Over 80% of sexually active people contract HPV at some point
- Transmission can occur even without visible warts
- Condoms reduce but don't eliminate risk
- Smoking weakens immune response to HPV
The World Health Organization confirms HPV as the most common sexually transmitted infection globally, with most infections clearing spontaneously within two years (WHO Fact Sheet).
Diagnosis Process: What to Expect
When evaluating potential 'cauliflower warts,' healthcare providers follow these steps:
- Visual examination - Most diagnoses happen through physical inspection
- Acetic acid test - Applying vinegar solution makes warts turn white
- Biopsy - For unusual growths or treatment-resistant cases
- HPV testing - Sometimes used with Pap tests for women
Self-diagnosis is unreliable—many skin conditions mimic genital warts. The American Sexual Health Association emphasizes that proper diagnosis requires professional medical evaluation (ASHA Resources).
Effective Treatment Options
While no treatment eliminates HPV completely, these approaches manage visible warts:
Medical Treatments
- Topical medications - Podofilox, imiquimod, or sinecatechins applied at home
- Cryotherapy - Freezing warts with liquid nitrogen (office procedure)
- Surgical removal - Excision, electrocautery, or laser treatment for larger clusters
Important Treatment Considerations
- Multiple treatments often needed for complete clearance
- Recurrence happens in about 30% of cases within 3 months
- Treatments work best when warts are small and few
- Immune health significantly impacts treatment success
Mayo Clinic research shows combination therapy (topical medication plus office procedures) yields the highest clearance rates (Mayo Clinic Guidelines).
Prevention Strategies That Actually Work
Reducing HPV risk requires multiple approaches:
Vaccination Effectiveness
The HPV vaccine protects against the strains causing genital warts. CDC data shows:
- 90% reduction in vaccine-type HPV infections since introduction
- 65% decrease in genital warts among vaccinated populations
- Maximum benefit when given before sexual debut (ages 11-12)
Practical Risk Reduction
- Maintain strong immune system through nutrition and sleep
- Limited sexual partners reduces exposure risk
- Regular STI screenings for sexually active adults
- Don't share personal items like towels or razors
When to Seek Immediate Medical Attention
Contact a healthcare provider if you notice:
- Bleeding from wart-like growths
- Rapid growth or color changes
- Pain during urination or intercourse
- Warts interfering with daily activities
- Recurrent outbreaks after treatment
While genital warts themselves aren't dangerous, similar-looking growths could indicate other conditions requiring different treatment approaches. The American Academy of Dermatology Association stresses that early intervention improves treatment outcomes (AAD Resources).
Common Misconceptions Clarified
Several myths persist about 'cauliflower warts':
- Myth: They always lead to cancer
Fact: Wart-causing HPV strains (6,11) differ from cancer-causing strains (16,18) - Myth: Home remedies like apple cider vinegar work
Fact: Unproven treatments can cause skin damage; medical guidance essential - Myth: Only sexually active people get them
Fact: HPV can spread through non-penetrative skin contact
Living with HPV: Long-Term Perspective
Most HPV infections clear within 1-2 years as the immune system eliminates the virus. The key considerations:
- Regular check-ups monitor for recurrence
- Stress management supports immune function
- Open communication with partners reduces transmission risk
- Vaccination protects against additional HPV strains
NHS UK reports that 90% of HPV infections resolve without treatment within two years, emphasizing the body's natural ability to clear the virus (NHS Genital Warts Information).
FAQ: Frequently Asked Questions
Can 'cauliflower warts' go away on their own?
Yes, approximately 20-30% of genital warts disappear without treatment within 3 months. However, waiting for spontaneous clearance increases transmission risk and allows warts to potentially grow larger.
Are 'cauliflower warts' contagious when treated?
Treatment reduces but doesn't eliminate contagion risk. The virus may remain in surrounding skin even after visible warts disappear. Consistent condom use and disclosure to partners remain important during and after treatment.
How long until 'cauliflower warts' appear after exposure?
The incubation period ranges from 2 weeks to 8 months, with most people developing visible warts within 2-3 months. Some never develop symptoms despite carrying the virus.
Can you get 'cauliflower warts' from toilet seats?
No, HPV requires direct skin-to-skin contact for transmission. The virus cannot survive long outside the human body, making transmission from surfaces like toilet seats extremely unlikely.











 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4